All things considered, I have a pretty regular menstrual cycle and like to track it on a period app. Yet, every month when my period comes around, it's as if I have lost all ability to function, and I worry about the cause. Menstruation isn't fun for anybody, but the week before my period begins is always horrendous. I'm slower, more forgetful, and I feel exhausted constantly.
I like to say that my attention-deficit/hyperactivity disorder (ADHD) meds feel like 'a drop in the ocean' around this time, but it's really better described as 'a drop in all the oceans combined' because those pills feel like they're doing nothing.
I mean, obviously, they do something, but it certainly doesn't feel like it.
❤️ Note from the editors: Menstruation (and the hormonal fluctuations that come with it) can affect anyone who menstruates, regardless of gender. While some of the studies cited are women-centric, this article uses gender-inclusive terminology whenever possible.
Too long; didn’t read
- It's not uncommon for ADHD symptoms to be worse during periods, or menstruation.
- It's possible that estrogen increases the effectiveness of stimulants, so low estrogen may dilute their effects.
- ADHD is a lifelong condition that can be affected by hormonal changes experienced through life.
Women, hormones, and ADHD
Recent research findings have revealed that women's ADHD symptoms are significantly influenced by hormonal changes and transitional periods, such as:
- Puberty
- Menstruation
- Pregnancy
- Postpartum
- Perimenopause
- Menopause
More specifically, lower levels of estradiol, an estrogen hormone, are associated with worsened ADHD symptoms. This is more prominent when progesterone or testosterone levels are already elevated, i.e., during cyclical hormonal changes.
Looking for extra support for your time of the month? The Inflow app has in-depth learning modules on many female-specific ADHD topics and a supportive community of ADHDers who really get it. Join us in the Inflow app!
Why is my ADHD worse during my period?
Many ADHDers report that their ADHD symptoms are worse during their periods. This is linked to decreases in estrogen and progesterone levels, which happens more than once during each cycle.
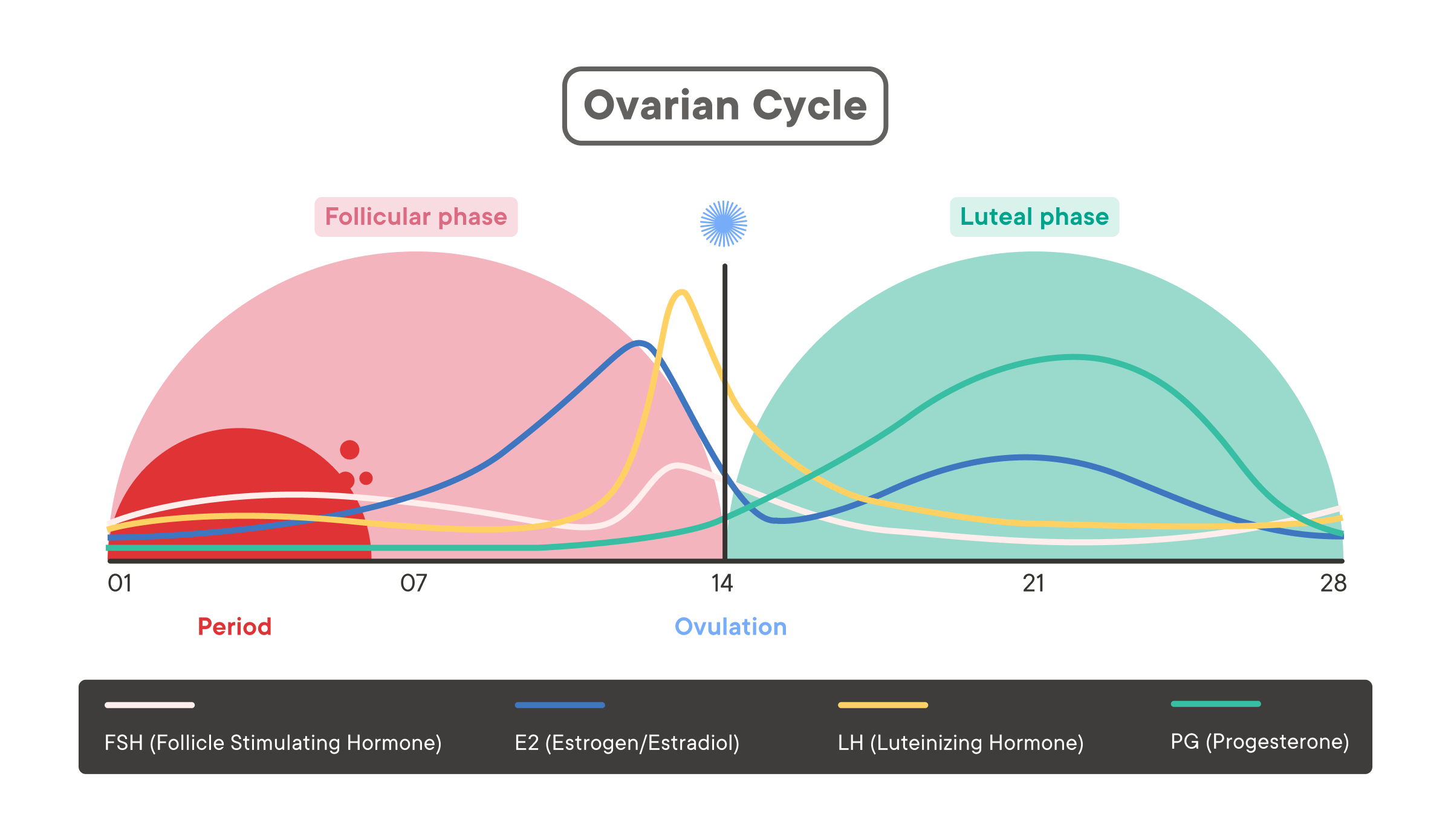
In a typical menstrual cycle, estrogen levels rise and fall twice:
- First rise: happens mid-follicular phase (just after menstruation)
- First fall: rapid; happens around ovulation (mid-cycle)
- Second rise: lower peak than the first rise; happens mid-luteal phase (after ovulation and before menstruation)
- Second fall: returns to baseline; happens at the end of the cycle, just before the next period
After the second drop, estrogen levels are at their lowest. These dips influence brain chemicals like dopamine, serotonin, and norepinephrine, affecting ADHD symptom severity.1
🩸 Period research! A 2017 study observed hormonal fluctuations and associated changes in ADHD symptoms. Researchers found that ADHD women who regularly struggle with impulsive behaviors tend to have less control over their impulses when estrogen levels drop. In other words, they were more impulsive on their periods. Additionally, the study found that ADHD symptoms vary throughout the menstrual cycle, with an increase observed during the early follicular and early luteal phases.2
ADHD and related reproductive health conditions

Can we all agree that experiencing a period is nothing like those tampon ads with people in white jeans leaping gleefully across open fields?
While some of us can still keep up with physical activity, others struggle with premenstrual syndrome (PMS) symptoms, such as:
- Cramps
- Tender breasts
- Headaches
- Bloating
- Constipation or diarrhea
Or you might experience a more extreme version of PMS, known as premenstrual dysphoric disorder (PMDD). PMDD can leave you with severe mood swings, high irritability, and worsening depression or anxiety.
🧠 ADHD research! A 2021 study on hormones and mood disorders found that women with ADHD experience severe PMS more often than those without ADHD.3 Researchers concluded that ADHD women might be more vulnerable to hormone-related mood disorders—PMDD, postpartum depression (PPD), and mood changes during pre- and perimenopause—during their lifetime.
Why does it feel like my ADHD medication isn't working during my period?
Stimulant-based medications are the most commonly prescribed treatment for ADHD. These are either methylphenidate-based (like Ritalin or Concerta) or amphetamine-based (like Adderall and Vyvanse.)
Amphetamine- and methylphenidate-based stimulants block the reuptake of dopamine and norepinephrine by neurotransmitter transporters in the brain. The amphetamine-based stimulants also block and slow down the release and reabsorption of dopamine and norepinephrine inside cells.
While it's still unclear what the chemical connection is between ADHD medication and menstruation, we can speculate that the rise and fall of estrogen may interfere with how well an ADHD drug works.
💊 Note: You can find more information on ADHD medication options in this article.
What can you do if this affects you?
The good news is that you're already here reading this; self-awareness is very important! The less-good news is that you'll need to consult a medical professional before significant changes can happen.
So, first things first - get your appointment scheduled! Next up, be ready to self-advocate by preparing questions for your appointment.
Talking points for your next doctor's visit
Write down some of these questions to address during your next appointment with your gynecologist and general practitioner.
- How do I track my menstrual cycle? Will it help me estimate when to expect a change in symptoms?
- Should I adjust my ADHD medication based on the time of the month?
- Can you tell me about hormonal contraception and how that might affect my ADHD and PMS symptoms?
- Do you recommend any lifestyle changes for particular times of the month so I can better manage my symptoms?
- What do you know about antidepressants and how they can affect my symptoms of PMS or PMDD (premenstrual dysphoric disorder)?4
Notes from our medical reviewer, OB-GYN
Hormonal contraceptives and ADHD medication: Potential interactions
Girls and young women with ADHD who take oral hormonal contraceptives (HCs) may have a three to six times higher risk of developing depression compared to neurotypical peers on similar birth control methods.
This finding has sparked controversy and requires further investigation.
Evidence-based treatment of PMS: SSRIs and the efficacy of combination oral contraceptives4
Selective Serotonin Reuptake Inhibitors (SSRIs) are widely recognized as an effective evidence-based treatment for PMS. Additionally, oral contraceptives have shown promising results in addressing PMS symptoms, particularly when combining drospirenone and ethinyl estradiol for a specific dosing regimen.
Clinical trials involving this combination, administered for 24 active days followed by four inactive days, have demonstrated a significant reduction in premenstrual symptoms compared to a placebo. This robust evidence underscores the potential benefits of this oral contraceptive approach in managing PMS.
-
Sources
1 Endocrinology of Female Reproduction | The Normal Menstrual Cycle and the Control of Ovulation (2018)
2 Psychoneuroendocrinology | Reproductive Steroids and ADHD Symptoms Across the Menstrual Cycle (2017)
3 Journal of Psychiatric Research | Prevalence of hormone-related mood disorder symptoms in women with ADHD (2021)
4 Journal of Clinical Psychiatry | Evidence-based treatment of Premenstrual Dysphoric Disorder: a concise review (2020)


.jpg)
.png)