Attention-deficit/hyperactivity disorder (ADHD) and obsessive-compulsive disorder (OCD) are common mental health conditions that share many similarities. ADHD and OCD are similar in that they are both affected by sensory input and genetics, and that they can both have an effect on focus and attention.
But there's more to it than that! Let’s explore both conditions and review the similarities and differences between the two.
Too long; didn't read
- The manifestations of ADHD and OCD are unique.
- The main difference between ADHD and obsessive-compulsive disorder lies in their classifications as mental health disorders: ADHD is a neurodevelopmental condition and OCD is an anxiety disorder.
- OCD obsessions can include thoughts about violence, perfectionism, sex, and germs, to name a few.
- OCD compulsions sooth obsessive thoughts, and a popular example is excessive cleaning.
What is obsessive-compulsive disorder?
When a person gets stuck in a cycle of obsessions and compulsions that adversely affect their quality of life, they may have OCD.
OCD obsessions
Obsessions are intrusive and unwanted thoughts, images, or urges that trigger uncomfortable feelings.
What do OCD obsessions look like?
- Contamination, germs, and illness
- Sexual acts
- Violence
- Religion, spirituality, and morality1
- Sexual and gender identity
- Relationships
- Perfectionism
- Death
OCD compulsions
Compulsions are behaviors that a person adopts to eliminate obsessions, or to soothe their stress and anxiety. More often than not, these behaviors develop without the person realizing it.
What do OCD compulsions look like?
- Excessive washing, cleaning, and scrubbing—sometimes more than 100 times per day
- Repeatedly checking on things or re-doing tasks, such as locking the door
- Counting while performing tasks to end on a “safe” number, such as "10" or an even number
- Excessive self-reassurance in order to quell anxious feelings
- Frequently asking others for reassurance - known as excessive reassurance-seeking (ERS)2
- Repeatedly rearranging items to keep them in a particular order
How common is OCD?
In the USA, 2.3% of adults have an official OCD diagnosis.3
Symptoms can appear at any age, but usually emerge between 10-18. According to the American Psychiatric Association (APA), OCD is more common in boys than girls during childhood, but shifts in adulthood and is slightly more prevalent in women than men.
OCD symptoms
OCD is an internalizing disorder, which means that the response to anxiety-inducing factors that are external are turned inward.
Common signs of OCD symptoms include:
- Inattention
- Obsessive or intrusive thoughts and behaviors
- Fear of harming self or others
- Excessive focus on order and symmetry
- Fear of losing (or not having) things
- Unwanted sexually-explicit or violent thoughts or images
- Fear of contamination
- Excessive concern with consequences of their actions
- Excessive focus on morality or religion
- Addictive tendencies
What is attention-deficit hyperactivity disorder?
ADHD is a neurodevelopmental condition with 3 presentations or subtypes: predominantly inattentive (ADHD-PI), hyperactive-impulsive (ADHD-HI), and combined type (ADHD-C).
All subtypes have the potential to interfere with work, school, relationships, and home life.
How common is ADHD?
9.4% of U.S. children are diagnosed with ADHD.
Boys have a higher rate of ADHD diagnosis at 12.9% (of all boys) compared to (all) girls at 5.6%.
In comparison, only 2.5% of American adults have ADHD. However, as mentioned in previous Inflow blogs, it's unlikely that these numbers are accurate due to insufficient data on ADHD adults, and previous gender bias in research studies.
ADHD symptoms
ADHD is an externalizing disorder that affects how people relate to their environment.
Common signs of ADHD include:
- Inattention
- Struggling to finish tasks
- Difficulty following directions
- Working memory deficits
- “Spacing out” without realizing
- Overlooking details that may lead ‘careless mistakes’
- Misplacing and losing items
- Forgetting appointments and missing deadlines
- Addictive tendencies
- Frequently interrupting or talking over others
- Socially inappropriate behaviors
ADHD vs. OCD
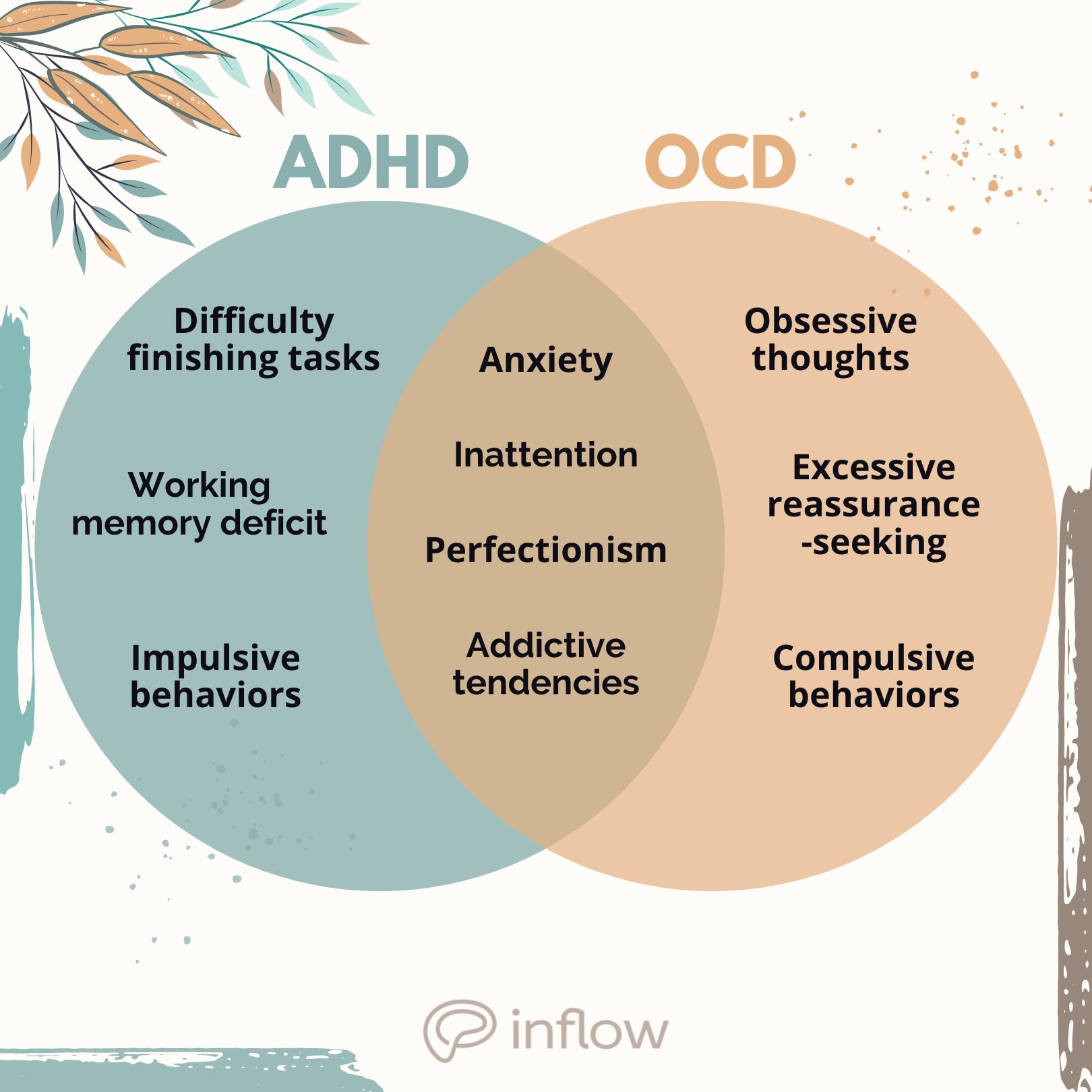
How are ADHD and OCD similar?
Shared causes
- Both may be caused by genetics, since they can run in families5,6
- Environmental exposures as a child
- Abnormal activity in the brain's neural frontostriatal system7, which is responsible for certain executive functioning skills, like motor control, cognition, and behavior
Shared traits and symptoms
- Anxiety
- Difficulty paying attention (likely due to dysregulated cognitive processing of incoming sensory information8)
- Perfectionism as a result of overcompensation for shortcomings (ADHD), or as an obsession (OCD)
- Hyperactivity as a diagnostic criterion (ADHD) or mimicked by certain compulsions (OCD)
- Addictive tendencies and prone to substance abuse9
How they're different...
Different classifications
- ADHD is an externalizing disorder, whereas OCD is an internalizing disorder.
- ADHD is a neurodevelopmental condition, and OCD is an anxiety condition.
Possibility of late-onset
- OCD can have a late onset (either naturally or in response to trauma10), but ADHD cannot* have a late onset (unless it's caused by traumatic brain injury, or TBI)
*this is not the same as ADHD symptoms becoming more obvious later in life due to ADHD masking or increased cognitive load. That can happen!
Can you have both ADHD and OCD?
Mental health conditions commonly co-occur with one another. In fact, a 2016 study found that 40.9% of people with OCD had ADHD symptoms as a child. For OCD adults, 16.9% reported ADHD symptoms.11
Coping strategies and treatment options
Coping strategies aren't one-size-fits-all, so it's unlikely that you will find an easy fix for your most difficult symptoms right away.
It's normal to try out a few strategies before finding a treatment or coping mechanism that works for you. In other words, don't give up! Review our suggestions below and discuss them with your doctor.
1. Self-care
One of the best coping strategies—for just about any ailment—is to maintain a healthy lifestyle. This can help reduce fatigue, anxiety, and depressive periods—all of which can exacerbate ADHD and OCD symptoms.
Try focusing on one or two of these habits:
- Switch to a healthier diet
- Exercise 4-7 days each week for 30 minutes (this can be light, like walking!)
- Limit screen time and social media to avoid blue light and anxiety triggers, respectively
- Try to get at least 7 hours of sleep each night12 (but we know sleep hygiene can be complicated for people with ADHD!)
- Create an ADHD-friendly routine, and try your best to stick to it
2. Cognitive behavioral therapy (CBT)
The goal of CBT is to strengthen or learn positive behaviors, and eliminate unwanted thoughts and behaviors. The sooner behavioral treatment can start, the more effective it is.
CBT for ADHD
A 2018 review concluded that CBT can help ADHDers manage inattentiveness, hyperactivity, and impulsive behaviors. Additionally, researchers found that CBT works best when combined with a medication regimen in order to reduce levels of anxiety.13
CBT for OCD
For OCD patients, CBT is used to break association between obsessive thoughts and compulsive behaviors. It also trains OCDers to avoid ritualizing when feeling anxious.
Specific therapies include exposure and response prevention (ERP), deep breathing exercises, progressive muscle relaxation, and cognitive restructuring.
3. Medications
Treating ADHD with stimulants
Stimulants are the most widely-used medication for ADHD. 70-80% of ADHD children have fewer symptoms when taking stimulants. Commonly prescribed stimulant brands include Adderall, Ritalin, Vyvanse, Dexedrine, Focalin, and Concerta.
Treating ADHD with nonstimulants and antidepressants
Non-stimulants have been used to treat ADHD since 2003.
Although they don’t work as quickly as stimulants, their effects can last 24 hours between doses. Some nonstimulants double as antidepressants. Commonly prescribed non-stimulant medications include Strattera, Kapvay, Intuniv, Tenex, Wellbutrin, Norpramin, Tofranil, and Aventyl.
Treating OCD with antidepressants
Antidepressants are the most effective medication for OCD symptoms.14
Brands commonly prescribed include Lexapro, Zoloft, Celexa, Prozac, Paxil, Anafranil, and Effexor. An additional drug, Cymbalta, may help OCD patients who do not respond to the other medications.
Deep transcranial magnetic stimulation
Deep transcranial magnetic stimulation is a non-invasive therapy approved by the FDA for the treatment of depression and some forms of OCD.
It utilizes magnetic fields to regulate the neural activity of brain structures, and can be combined with other forms of therapy. It has no known adverse side effects.
Frequently asked questions: obsessive-compulsive disorder & ADHD
What are the main differences between ADHD and OCD?
While both are mental health conditions, they belong in separate subcategories. ADHD is an externalizing neurodevelopmental disorder, and OCD is an internalizing anxiety disorder.
How are ADHD and OCD similar?
People with ADHD and people with OCD share a few common traits, such as anxiety, perfectionist tendencies2, and difficulty paying attention (with or without hyperactivity).8 The last one is especially likely in environments with lots of stimuli.
Can someone have both ADHD and OCD?
Yes! OCD and ADHD frequently co-occur with one another.11 These are called comorbidities or comorbid conditions.
How are ADHD and OCD treated?
Both conditions can be managed with medication, therapy, and lifestyle adjustments; however, effectiveness of treatment varies from person to person. The most common routes involve a combination of therapy and medication.13,14
Can trauma cause OCD?
Yes! Traumatic experiences have the potential to trigger obsessions centered around the trauma, which may result in unhealthy compulsions.10







